History of Schizophrenia: Then vs. Now

Considered one of the most serious and debilitating mental illnesses, schizophrenia is broadly described as a a long-term brain disorder in which individuals interpret reality abnormally. Symptoms of schizophrenia are complex and varied, ranging from cognitive impairments such as mental confusion to physical manifestations like catatonia. Although the illness was not thoroughly researched until the early 20th century, official medical accounts of similar symptoms have been reported from as early as the late 1700's. Kurt Schneider was the first psychiatrist to officially create a list of traits, called first-rank symptoms, than distinguished Schizophrenia from other mental illnesses. His research greatly contributed to all that we know today concerning this illness, but some aspects of his theory have since been questioned in today's medical community.
It was not until 1908 that Dr. Eugen Bleuler coined the term schizophrenia, which translates to "splitting of the mind" in Greek, to describe this rare illness. He was one of the first medical professionals whose patients showed marked improvement under his care as opposed to the hundreds of others at the time who seemed to deteriorate over time. He described schizophrenia's symptoms using the 4 A's model. He believed that the symptoms could be filed into four categories: Flattened Affect, Autism, impaired Association, and Ambivalence. Using Dr. Bleuler's model, the treatment of schizophrenia dramatically improved and was further boosted with the development of Chlorpromazine in the 1950's, one of the first pharmacological agents that showed results in those living with schizophrenia.
With increasing technology and awareness of mental illness, there has been a mass increase in research concerning schizophrenia and how to help those diagnosed with the disease. The DSM-V now has detailed information describing the symptoms and diagnosis of the schizophrenia spectrum which includes schizophrenia, schizo-affective, and delusional disorder. The different categories allow for a more accurate diagnosis as this particular mental illness differs in severity from person to person. The DSM-V describes the symptoms for schizophrenia as follows:
It was not until 1908 that Dr. Eugen Bleuler coined the term schizophrenia, which translates to "splitting of the mind" in Greek, to describe this rare illness. He was one of the first medical professionals whose patients showed marked improvement under his care as opposed to the hundreds of others at the time who seemed to deteriorate over time. He described schizophrenia's symptoms using the 4 A's model. He believed that the symptoms could be filed into four categories: Flattened Affect, Autism, impaired Association, and Ambivalence. Using Dr. Bleuler's model, the treatment of schizophrenia dramatically improved and was further boosted with the development of Chlorpromazine in the 1950's, one of the first pharmacological agents that showed results in those living with schizophrenia.
With increasing technology and awareness of mental illness, there has been a mass increase in research concerning schizophrenia and how to help those diagnosed with the disease. The DSM-V now has detailed information describing the symptoms and diagnosis of the schizophrenia spectrum which includes schizophrenia, schizo-affective, and delusional disorder. The different categories allow for a more accurate diagnosis as this particular mental illness differs in severity from person to person. The DSM-V describes the symptoms for schizophrenia as follows:
"Schizophrenia is characterized by delusions, hallucinations, disorganized speech and behavior,
and other symptoms that cause social or occupational dysfunction. For a diagnosis,
symptoms must have been present for six months and include at least one month of active symptoms."
and other symptoms that cause social or occupational dysfunction. For a diagnosis,
symptoms must have been present for six months and include at least one month of active symptoms."
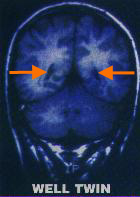
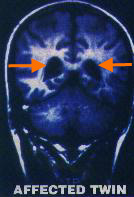
In addition to a more concrete and objective definition of schizophrenia, modern technology has presented a possible cause of this illness as well. Multiple research studies have found a strong correlation between genes and risk of developing schizophrenia. The study suggests that the more cases of the illness in families, the higher the chances of one developing the schizophrenia. Other studies have also found biological differences in brain functioning between those with schizophrenia and individuals with no preexisting psychological problems. The NIMH suggests that "fluid-filled cavities at the center of the brain, called ventricles, are larger in some people with schizophrenia. The brains of people with the illness also tend to have less gray matter, and some areas of the brain may have less or more activity" which adds a biological element to the illness. Many psychologists regard schizophrenia as a sort of threshold which can be surpassed by genetic, biological, and environmental influences.
|
A graph representing the correlation between genetics
and the risk of developing schizophrenia. The results indicate a strong genetic role in this illness. |
Representation of the differences in ventricle size
as well as grey matter in two identical twins, one of which is diagnosed with schizophrenia. |
For more information about schizophrenia, go to the following links:
http://www.nimh.nih.gov/health/topics/schizophrenia/index.shtml#part_145426
http://www.amhc.org/1418-dsm-5/article/51960-the-new-dsm-5-schizophrenia-spectrum-and-other-psychotic-disorders
http://www.mariayang.org/2013/08/28/dsm-5-schizophrenia/
http://www.dsm5.org/Documents/Schizophrenia%20fact%20Sheet.pdf